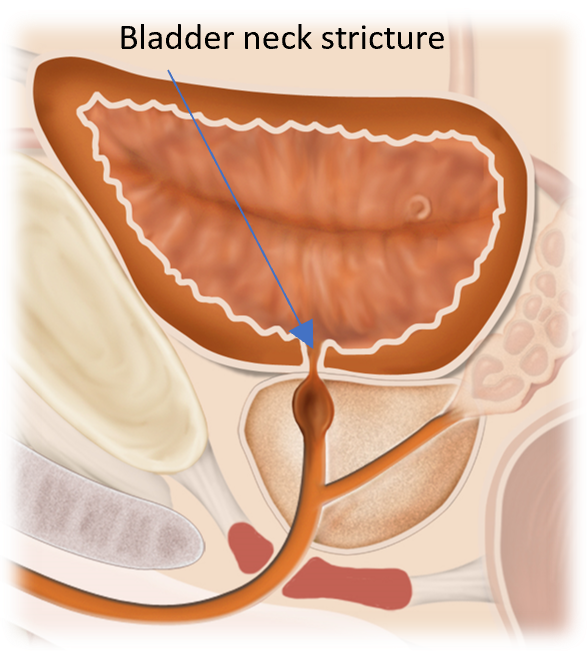
What is Bladder Neck Stricture?
How Bladder Neck Stricture Affects Urine Flow
Bladder Neck Stricture in the Urinary System
The kidneys produce urine, which is transported to the urinary bladder. The bladder stores urine until it is emptied through the urethra during urination. For normal urine flow to occur, the opening between the bladder and the urethra, known as the bladder neck, must remain unobstructed.
Bladder neck stricture is a condition in which this opening becomes narrowed, restricting the flow of urine from the bladder. This narrowing can interfere with normal bladder emptying and may lead to urinary symptoms that require medical intervention to avoid patient complications.
Symptoms of Bladder Neck Stricture
- Difficulty starting urination
- Weak or interrupted urine stream
- A feeling of incomplete bladder emptying
- Increased need to urinate, especially at night
- Straining during urination
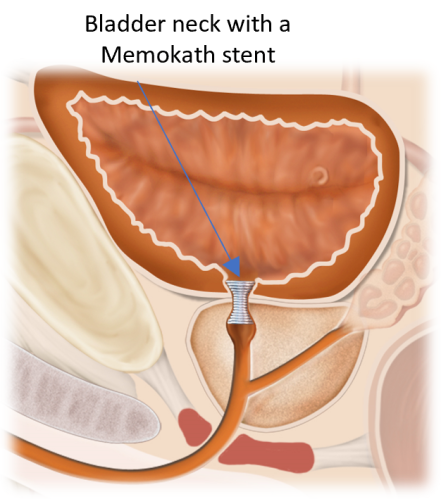
The Memokath™ solution
Memokath™ is a long-term solution for men who are not able nor wish to go through often repeated procedures or major surgery.
Memokath™ is a supportive spiral tube made of nickel-titanium ”Ni-Ti” which is inserted in the urethra to re-create passage of the urine.
Memokath™ is inserted under local anaesthesia and the stent is carefully inserted through the penis and placed with a cystoscope. The insertion usually takes about 30-40 minutes. After the insertion it is advised to drink plenty of water to minimize the risk of cystitis. Most patients can leave the hospital the same day and return to their daily routines.
Memokath™ is designed as a long-term solution and it can be left in place for several years
Memokath™ does not activate security alarms. Since it is CT- and MRI compatible getting a scan is no problem. It does not cause nickel allergy as there is no nickel on the stent surface.