What is Ureteric Stricture?
How Ureteric Stricture Affects Urine Flow
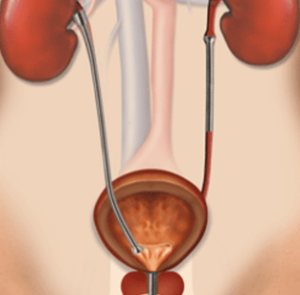
How Ureteric Stricture Affects Urine Flow
The kidneys produce urine which is carried to the bladder by a fine muscular tube called a ureter. The urinary bladder acts as a reservoir for the urine and, when it is full, it is emptied via the urethra (urination). The urine relieves the body from unwanted substances, and it is essential that urine can leave the body freely.
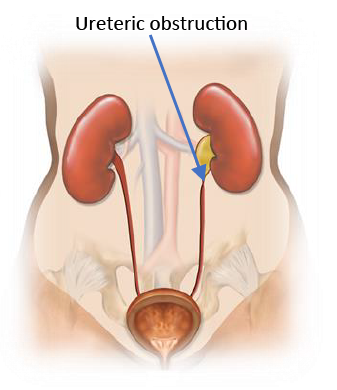
A ureteric obstruction is an abnormal narrowing of the ureter blocking the passage of urine through the ureter. An obstruction of the ureter can lead to reduced kidney function as well as infection.
Ureteric Obstructions
The most common symptoms are constant or intermittent flank pain/lower abdominal pain. Other symptoms can be:
- General discomfort, fever and nausea
- Urinary tract infection
- Foul-smelling urine
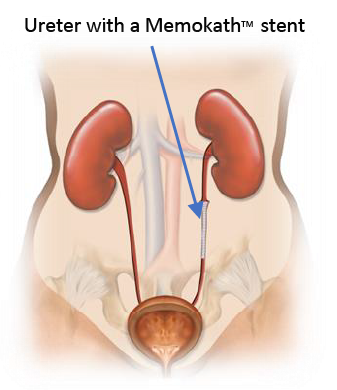
The Memokath™ solution
Memokath™ is a long-term solution for men and women of all ages who are not able nor wish to go through often repeated procedures or major surgery and aiming for a better quality of life.
Memokath™ is a supportive spiral tube made of nickel-titanium ”Ni-Ti” which is inserted in the ureter to recreate a passage for the urine through the ureter. It is passed through the urethra into the bladder and up into the ureter. The Memokath™ stent covers only the obstruction and not the healthy part of ureter. The procedure is performed under general or spinal anaesthesia and it
normally takes approximately 40-50 minutes.
After the insertion, it is advised to drink plenty of water as it minimizes the risk of urinary tract infection. Most patients can leave the hospital on the day of treatment and return to their daily routines within a few days.
Memokath™ can be left in place for several years as it is designed as a long-term solution. It does not activate security alarms and since it is CT and MRI compatible getting a scan is no problem. It does not cause nickel allergy as there is no nickel on the stent surface.